Pain in the front of the knee and around the patella (i.e. the kneecap) is a common occurrence in the growing child as well as in the adolescent years. There are numerous factors that contribute to the development of this pain syndrome, but only rarely does it result directly from a specific injury. Severity also varies widely among patients: from involvement only with vigorous sports participation to affecting activities of daily living such as sitting for prolonged periods of time, going up and down stairs, and/or the simple task of walking around school. Because this pain originates from the patella-femoral joint of the knee, it is commonly called Patella-Femoral Pain Syndrome (PFPS). A more technical term is Chondromalaica Patella (chondro = cartilage, malacia = softening).
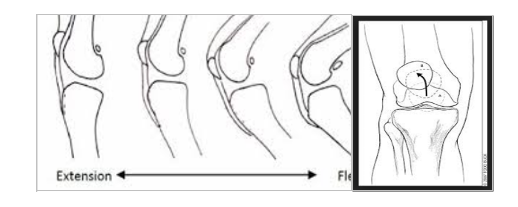
Chondromalacia Patella results from micro-instability of the patella. When the knee is extended (i.e. straight), the patella is mobile. When flexing (i.e. bending) the knee, the patella has to find a groove in the femoral (the sulcus). In PFPS, the patella does not track perfectly and is sloppy in going down the femoral sulcus. Over thousands and thousands of cycles, this maltracking softens the articular cartilage on the undersurface of the patella. This produces a dull, but sometimes sharp, pain in front of the knee and around the patella. The severity is inversely proportional to the level of activity of the knee (i.e. pain with less activity is more severe involvement).
Factors that contribute to the development of Chondromalacia Patella include:
-
Muscle Imbalance – With growth, certain muscles (like the Quads and Hamstrings) get tight, putting more pressure on the patella. Additionally, the patella (as it lives within the Quadriceps’ mechanism) is pulled in different directions by different muscles.
-
Overuse – It makes sense that excessive repetitive activities lead to “over-doing-it”.
-
Deconditioning – Just the opposite of overuse is deconditioning. After an injury, or surgery, the muscles of the lower extremity may be weaker than they were before, exacerbating the muscle imbalance previously mentioned.
-
Mechanical factors – Ligamentous laxity, rotational anomalies of the lower extremities, patella alta (high riding patella), or knock knees are some of the structural contributing factors.
Treatment depends on the severity and duration of symptoms. Rest from excessive activities is paramount to control pain. Anti-inflammatories and over-the-counter neoprene knee sleeves are temporary measures to reducing the pain, and may allow partial return to some sports. However, the most definitive treatment comes with the guidance of a Physical Therapist to instruct the patient on a home program to stretch tight tendons and/or condition muscles.
